If you or someone you know has been diagnosed with glaucoma, you likely want to learn more about this eye condition. Between speaking with your doctor and researching glaucoma and various treatment options online, there is plenty of information available. If you are curious and want to learn even more about this progressive disease that affects millions of people in the United States, we are here to help!
If you or someone you know has been diagnosed with glaucoma, you likely want to learn more about this eye condition. Between speaking with your doctor and researching glaucoma and various treatment options online, there is plenty of information available. If you are curious and want to learn even more about this progressive disease that affects millions of people in the United States, we are here to help!
In part one of our Glaucoma 101 blog series, we are highlighting some important information about this condition, including the various types of glaucoma, symptoms, potential causes, and potential demographics.
What Is Glaucoma and What Are the Different Types?
If you have been recently diagnosed with glaucoma, you are not alone! Statistics show that this eye condition affects nearly 3 million people over the age of 40 in the United States. Glaucoma is a progressive eye disease that causes damage to the optic nerve and is often associated with increased pressure in the eye due to an imbalance in production and outflow of ocular fluid. In a healthy eye, fluid is produced to help maintain the eye’s shape. Normally, this natural fluid flows out through an area called the trabecular meshwork and is absorbed into the bloodstream. However, for someone with glaucoma, the fluid does not drain at the same rate that it is produced, causing pressure to build in the eye. Over time, this increased pressure can damage the optic nerve and impact vision.
Glaucoma is the second leading cause of blindness worldwide and the effects of the condition are irreversible. If you have glaucoma, it is important to keep up with your regularly scheduled eye visits and treatment, as the condition can lead to vision loss. You may not know this, but there are actually a few different types of glaucoma.
Open-Angle Glaucoma
The most common type of glaucoma is called open-angle glaucoma. It accounts for about 70-90% of cases. Open-angle glaucoma can occur when the drainage angle formed by the cornea remains open and the trabecular meshwork is partially blocked, causing the pressure in the eye to increase and eventually damage the optic nerve. There are typically no warning signs or symptoms to indicate that you might have open-angle glaucoma. This type of glaucoma can develop slowly over time and may go unnoticed, especially if vision only changes slightly. Often during the aging process, the trabecular meshwork starts to decline in function, affecting how the fluid flows throughout the eye.
If you are diagnosed with open-angle glaucoma and do not seek treatment, the pressure in the eye can increase and continue to build. This can gradually lead to loss of peripheral vision and blindness, so it’s particularly important to speak to your doctor and identify a treatment plan.
Angle-Closure Glaucoma
Angle-closure glaucoma, also referred to as narrow-angle glaucoma, is the second most common type of glaucoma. This tends to occur when the iris bulges forward, blocking the drainage angle formed by the cornea and iris. With this type of glaucoma, you may feel eye pain and experience hazy or blurred vision. These symptoms can occur because the build-up and increased pressure cause the fluid in the eye to not circulate properly.
Angle-closure glaucoma can occur suddenly or gradually. If you find that your glaucoma has occurred suddenly, it may be considered acute angle-closure glaucoma. However, if it is progressing gradually, the condition is more specifically referred to as chronic angle-closure glaucoma. Speak with your doctor to learn more.
Normal-Tension Glaucoma
With normal-tension glaucoma, also known as low-tension or normal-pressure glaucoma, the optic nerve becomes damaged even though eye pressure is within a “normal” range. This condition may occur due to a sensitive optic nerve or reduced blood supply to the optic nerve, which is caused by the hardening of the arteries.
What Are the Symptoms of Glaucoma and How Do You Test for It?
 Now that you know about the different types of glaucoma, you’re likely wondering what symptoms could indicate you or a loved one may be living with this progressive condition. It is very important to know that people who are diagnosed with glaucoma often don’t experience symptoms. If you do develop symptoms, they may vary depending on the type of glaucoma you have and how advanced the condition is. Since there are often little to no symptoms of glaucoma, it’s important to keep your regularly scheduled eye exams to catch glaucoma before it affects your vision. If you are experiencing any potential symptoms, you should make an appointment with your eye doctor.
Now that you know about the different types of glaucoma, you’re likely wondering what symptoms could indicate you or a loved one may be living with this progressive condition. It is very important to know that people who are diagnosed with glaucoma often don’t experience symptoms. If you do develop symptoms, they may vary depending on the type of glaucoma you have and how advanced the condition is. Since there are often little to no symptoms of glaucoma, it’s important to keep your regularly scheduled eye exams to catch glaucoma before it affects your vision. If you are experiencing any potential symptoms, you should make an appointment with your eye doctor.
Below are some possible symptoms that may indicate you or someone you know is living with glaucoma:
- Frequent, patchy blind spots in peripheral or central vision
- Severe headaches
- Pain in eyes and forehead
- Nausea
- Vomiting
- Seeing rainbows or halos around light
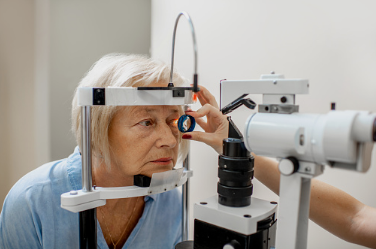
If you notice any changes in your vision or have experienced any of these symptoms, you may be wondering what to expect if you schedule an eye exam. Don’t worry we’ve got you covered! Your doctor will likely perform the following procedures and/or tests to check for glaucoma:
- Measure eye pressure
- Visual field test, to see if your peripheral vision is worsening
- Examine your eye’s drainage angle
- Test side vision
- Gonioscopy, which evaluates the eye’s drainage system
- Ultrasound Biomicroscopy, a technique used for imaging the eye
- Take a detailed picture of your optic nerve
- Measure the thickness of your cornea
During an eye exam, you can also learn more information from your doctor by asking him or her any questions you may have about glaucoma, including symptoms or risks.
What Are the Causes and Risk Factors of Glaucoma?
 There are various causes and risk factors of glaucoma to be aware of. Gaining knowledge and insight into these may help you or a loved one determine if you need to have an eye exam or be tested for glaucoma. Below, you will find some causes and risk factors that could help you learn more about your glaucoma diagnosis or your chance of developing this condition.
There are various causes and risk factors of glaucoma to be aware of. Gaining knowledge and insight into these may help you or a loved one determine if you need to have an eye exam or be tested for glaucoma. Below, you will find some causes and risk factors that could help you learn more about your glaucoma diagnosis or your chance of developing this condition.
Risk Factors
Certain demographics may put you at an increased risk of developing glaucoma. While anyone can develop glaucoma, some populations are more at-risk than others. Based on your affiliation to the demographics below, your eye doctor will be able to determine how often you should schedule eye exams.
- African Americans: African American populations and those of African descent have a higher risk of developing glaucoma. Glaucoma is six to eight times more common in African Americans than in Caucasians.
- Anyone Over the Age of 60: People over the age of 60 possess an elevated risk and are six times more likely to have glaucoma.
- People With a Family History: If there are members in your immediate family that have glaucoma, your chances of developing the condition are higher. If this is the case, it’s important to stay in contact with your eye care professional and get screened regularly.
- Hispanic Groups: Studies show that Hispanics over the age of 60 are at a greater risk of developing glaucoma.
- Asian Populations: Those of Asian descent have an increased risk of angle-closure glaucoma, and people of Japanese descent are even more likely to be diagnosed with normal-tension glaucoma.
Potential Causes
If you have been recently diagnosed with glaucoma, you might be wondering how you developed this eye condition. Well, there are a few different potential causes that might help answer your question. In fact, the higher your eye pressure is, the higher the risk of damage to your optic nerve. Some causes of glaucoma include:
- Elevated eye pressure: When eye fluid is produced and does not drain normally through the trabecular meshwork, a build-up of a fluid called aqueous humor flows through the inside of your eye, which causes eye pressure to increase.
- Blunt eye trauma: This can result in immediate increased eye pressure or cause internal damage.
Inflammatory eye conditions, such as Uveitis.
Gaining Insight Into Glaucoma
Now that you know more about the types, causes, symptoms, and risk factors of glaucoma, hopefully, you have a better understanding of the condition. Having this additional insight can help you learn a little bit more about your or a loved one’s diagnosis, or help determine if you may be at higher risk of developing the condition. If you have any questions about glaucoma or available treatment options, don’t hesitate to reach out to your doctor. You can also visit our website to learn more or to hear from others who have shared their experience with glaucoma.
Stay tuned for Part Two of our Glaucoma 101 blog series, where we will discuss treatment options, such as iStent inject® W, and post-treatment care. Don’t forget to follow Living with Glaucoma on Facebook, Twitter, and Instagram.
PM—0098 Rev 1